
By Miriam Raftery
Photo: Creative Commons via Bing
April 18, 2020 (El Cajon) – COVID-19 is having a devasting impact on nursing home patients. Nationwide, over 7,000 nursing home-related deaths have occurred, the New York Times reported on Friday in a headline that referred to the facilities as “death pits.”
Today, the California Health Department for the first time released statistics on coronavirus cases in nursing facilities. Locally, the hardest hit area is El Cajon, where 42 patients have been diagnosed with the virus in three nursing homes: Country Hills Post Acute (19), Bradley Court (12), and Avocado Post Acute (11).
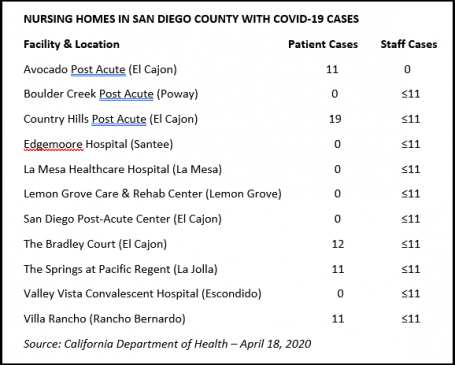 Staff cases have been reported at 10 facilities in San Diego County, including La Mesa Healthcare and Lemon Grove Care & Rehab Center. The state’s database indicates each facility had fewer than 11 cases as of the reporting deadline yesterday. There are also patient cases at two other San Diego area facilities in La Jolla and Escondido.
Staff cases have been reported at 10 facilities in San Diego County, including La Mesa Healthcare and Lemon Grove Care & Rehab Center. The state’s database indicates each facility had fewer than 11 cases as of the reporting deadline yesterday. There are also patient cases at two other San Diego area facilities in La Jolla and Escondido.
A full list of all facilities in the state and county reporting positive cases is available here, however the list includes only nursing homes and does not include other senior facilities such as retirement centers or assisted living homes.
Of those facilities that did report, there are 1,290 patient cases and 1,740 staff cases statewide to date.
The Centers for Disease Control has published guidelines for nursing homes and long-term care facilities, aimed at reducing spread of the disease among vulnerable elderly patients, many with pre-existing conditions.
The COVID-19 public health orders in California prohibit visitors at such facilities, leaving elderly patients to contend with the mental stress of isolation in addition to any physical or cognitive impairments, also putting severe stress on families and caregivers.
“We don’t have what we need to stop this,” Mark Parkinson, the president and chief executive of the American Health Care Association and the National Center for Assisted Living, told the New York Times. “We have got to have masks, and we don’t have masks.”
He added that federal health authorities have designated nursing homes and long-term care facilities at a lower priority level than hospitals, meaning longer turnaround times for test results that could slow the spread. In addition, Parkinson concluded, many employees in nursing facilities do not have the option of isolating themselves from patients who are ill.













Recent comments