 By Helen L. Horvath
By Helen L. Horvath Captain Smith: I actually started out with a life plan of being a PhD scientist in science and math, so I first pursued economics. After graduating with my bachelor’s degree in economics, I began interviewing with banks and other industries – in the end they did not appeal to me. I wanted to fly airplanes and decided to join the military and was interested in flying on aircraft carriers, so I spoke to the Navy recruiter and the Navy decided to let me fly. I went to aviation flight school. Eventually, I realized that I wanted to do something else to help the community, so I went on to get my master’s degree in cellular and microbiology in preparation to become a board certified pediatrician.
Captain Smith: I actually started out with a life plan of being a PhD scientist in science and math, so I first pursued economics. After graduating with my bachelor’s degree in economics, I began interviewing with banks and other industries – in the end they did not appeal to me. I wanted to fly airplanes and decided to join the military and was interested in flying on aircraft carriers, so I spoke to the Navy recruiter and the Navy decided to let me fly. I went to aviation flight school. Eventually, I realized that I wanted to do something else to help the community, so I went on to get my master’s degree in cellular and microbiology in preparation to become a board certified pediatrician. 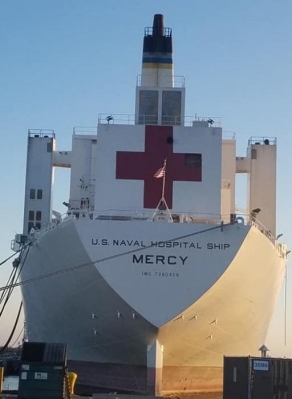 ECM: In researching the San Diego Naval Medical Center’s service delivery area, the research showed that your facility is responsible for the ships assigned to San Diego when in port for medical and dental care. This includes the USNS Mercy. In March 2020, the Mercy was sent to Los Angeles to permit non-military and VA hospitals to lighten the load of civilian medical centers. Where did the Mercy obtain its staff for deployment?
ECM: In researching the San Diego Naval Medical Center’s service delivery area, the research showed that your facility is responsible for the ships assigned to San Diego when in port for medical and dental care. This includes the USNS Mercy. In March 2020, the Mercy was sent to Los Angeles to permit non-military and VA hospitals to lighten the load of civilian medical centers. Where did the Mercy obtain its staff for deployment? In addition, the Medical Center looks different and is restricted to one of three entry points with the overall footprint looking different. Anyone entering the hospital will have a temperature check. This minimizes employee and patient risk. The hospital has separated the Fleet mission and Fleet members from the general authorized healthcare patients. Patients who believe they have COVID-19 are directed to the COVID-19 tent for testing. The tent is fully wired (with technology and medical equipment) to care for the needs of the potentially infected patient.
In addition, the Medical Center looks different and is restricted to one of three entry points with the overall footprint looking different. Anyone entering the hospital will have a temperature check. This minimizes employee and patient risk. The hospital has separated the Fleet mission and Fleet members from the general authorized healthcare patients. Patients who believe they have COVID-19 are directed to the COVID-19 tent for testing. The tent is fully wired (with technology and medical equipment) to care for the needs of the potentially infected patient.
 ECM: Since COVID-19 is a virus without an immunization or cure currently available along with the fact that the virus mutates as it spreads, what has been the treatment method for the virus at the Medical Center?
ECM: Since COVID-19 is a virus without an immunization or cure currently available along with the fact that the virus mutates as it spreads, what has been the treatment method for the virus at the Medical Center?
Captain Smith: The majority of the infected do not require hospitalization and are managed from a home care setting. The spread of COVID-19 has no common thread. Science is attempting to do in 20 months what normally takes years of research and development. It is possible that science has not caught up with facts.
ECM: Are there any specific general or specialty clinics that are currently unable to operate due to COVID-19?
Captain Smith: The Medical Center is pretty much doing now what was previously done in a pre-COVID-19 medical environment. Services have not been cut down as the various medical clinics continue to operate. The Naval Medical Center, San Diego is a tertiary (regional) medical center (for the military and veterans) – we do just about anything. The first month of the pandemic, the entire health system shut down. Currently the Naval Medical Center San Diego has no (major) issues as services continued (throughout the pandemic). At the same time, one of the key factors that need to be worked on is the backlog of services, surgeries, and how the Medical Center will address the global healthcare issues. The Naval Medical Center San Diego needs time.
ECM: With the need for round the clock childcare for medical staff, how is your medical center responding to employees’ childcare needs or lack of childcare during this pandemic? This is based upon the fact that much of the overall military childcare system is either shut down or has reduced service hours according to discussions with Navy childcare facilities. Has this been considered in the phase in plan for employees?
Captain Smith: As a pediatrician, I can say that a child’s job is to find viruses and spread the germs. This is what happens in childcare centers creating a need to monitor the installation childcare facilities. The Navy is aware of the need for employee childcare and is working with staff to address the reduction in available childcare services on the installation.
ECM: Based upon the current modifications to medical operations, will the hospital continue to operate using the modifications (i.e. telehealth/medicine appointment, teleworks, and other innovations) to maintain your current workforce? Also, will the Navy continue to operate utilizing the current modifications to healthcare delivery and employee engagement?
Captain Smith: As we are a medical center, we have begun to use telemedicine and virtual appointments for care not requiring face to face appointment. This includes mental health, primary care, and other services.
ECM: How can the active duty, veteran and family members support the Medical Center’s efforts to continue healthcare while in the COVID-19 environment?
Captain Smith: Stay informed through official websites and social media. When a person is sick, go to the hospital to be seen. A lot of authorized patients think they cannot go to the hospital. Nothing is worse than having a mild illness and not receiving treatment and become more ill.
ECM: What can we, as a community do better in both healthcare and life in general?
Captain Smith: Do better? I do not (specifically) know because there is so much that we do not know about the virus and how it behaves. There are a lot of intelligent people providing advice. Yet, we needs to have a consensus in the advice. The current guidelines are easy to follow (mask, social distancing, etc).
ECM: Thank you for your time. Is there anything else you would like to let the community know?
Captain Smith: Naval Medical Center, San Diego is here and ready to take care of you. Use telehealth and other services available. Let us get the message out there that we (Naval Medical Center, San Diego) are open. Do not be shy, much (of healthcare) can be done virtually. We would love to have you come in and receive care in our world.
NOTE: Naval Medical Center, San Diego is open to active duty personnel, their authorized family members (i.e. spouses and children), veterans and their authorized family members, and at times provided emergency treatment through cooperative agreements in the San Diego community such as the Veterans Administration.
*The Naval Hospital San Diego is a 1.2 million square foot medical center. It has 18 operating rooms, two Fisher House Homes, a 250-seat auditorium, a 200 seat chapel, and a medical and surgical simulation center used to teach aspiring doctors and medical staff. On an average day, the Naval Medical Center completes 44 operating room cases, has 45 inpatient admissions, and will deliver six babies. Naval Medical Center also has a neonatal intensive care unit for premature babies. On any day, the Naval Medical Center, San Diego generally will fill 6,500 prescriptions, have 5,800 patient visits, 200 emergency visits a day, while managing a cadre of graduate medical students and sharing resources through cooperative agreements with the Veterans Administration and other healthcare facilities
UCSD and the VA have a medical fellowship cooperative agreement program for most major medical specialties. Additionally, the VA and Naval Medical Center have cooperative research and development agreements with government, universities, and industries.
Dr. Helen Horvath is an Army veteran, published author, psychologist, and organizational development consultant. As a speaker, she has been invited to speak at the American Psychological Association Annual Conference, Society of Industrial and Organizational Psychology, and other key professional organizations.
 Dr. Horvath is a published author on a variety of psychology and business-related topics. She is a former marriage and family therapist who also published a relationship book entitled “Put a Period to IT: When Divorce is the Option.”
Dr. Horvath is a published author on a variety of psychology and business-related topics. She is a former marriage and family therapist who also published a relationship book entitled “Put a Period to IT: When Divorce is the Option.”
East County Magazine gratefully thanks the Facebook Journalism Project for support through its COVID-19 Local News Relief Fund Grant Program to help make this reporting possible. #FacebookJournalismProject.
You can donate to support our local journalism efforts during the pandemic at https://www.EastCountyMedia.org/donate.









Recent comments